Recently Diagnosed
Diagnosis
If any abnormalities are detected in the prostate during the DRE, or if PSA levels are higher than normal or are rising, the doctor may recommend further testing.
Urine test
Urine is analyzed for abnormalities that may indicate a problem other than prostate cancer, such as bacterial infection, or to rule out conditions that may cause the same signs and symptoms of prostate cancer, such as prostatitis (inflammation of the prostate) and benign prostatic hyperplasia (enlarged prostate).
Transrectal Ultrasound
This procedure uses sound waves to visualize the prostate gland and detect any abnormalities.
Transrectal Power Doppler Ultrasound (also known as Doppler scan)
This procedure is similar to the transrectal ultrasound, but a Doppler shift measures blood flow and resistance levels in veins and arteries. The rapid flow of blood through tiny blood vessels that are characteristic of tumors can be observed. Currently, there are very few Doppler scans in clinical use. Ultrasounds help in diagnosing, staging, and treatment plans by measuring prostate gland volume, recognizing varied patterns of cancer, and identifying appropriate sites for biopsy. Ultrasonography alone, however, cannot detect all cancer If these test results indicate the presence of prostate cancer, the next step is a prostate biopsy. A biopsy is a procedure in which small tissue samples from the prostate are collected and sent to a pathologist for analysis. Biopsy results are usually obtainable within 10 days. Two kinds of biopsies are generally performed – transrectal or transperineal. Transrectal is the most common. An enema and an oral antibiotic are often given prior to the biopsy. Local anesthesia is rarely used. The doctor will insert an ultrasound probe into the rectum. The probe will visualize images to guide the doctor to abnormal areas of the prostate. From outside the rectum wall, a handheld device with a spring-loaded, slender needle is positioned and inserted into the abnormal areas to collect tissue samples. If no abnormal areas are detected, various tissue samples are collected from different areas of the prostate. The transperineal procedure is the same as the transrectal procedure, only the needle is inserted through the skin between the rectum and scrotum (perineum). This method is used when access through the rectum wall is not possible. If cancer is present, the doctor (urologist) will assess the stage of the cancer and how fast it is likely to grow. The doctor may decide to run further tests to determine if the cancer has spread to other tissues in the body.
Bone scan
Detects whether the cancer has spread to the bones.
Ultrasound
Detects whether the disease has spread to nearby tissues.
Chest X-ray
Shows whether the cancer has spread to the lungs, ribs, or backbone.
Computerized tomography (CT) scan
Identifies general signs of disease, such as enlarged lymph nodes* or organ abnormalities that may be related to prostate cancer.
Magnetic resonance imaging (MRI)
Detects spread of cancer to lymph nodes and bones.
Lymph node biopsy
Determines whether the cancer has spread to the lymph nodes. *Lymph nodes are small glands located in many parts of the body that help defend against harmful foreign particles. Lymph nodes in the pelvic region are usually the first place to which cancer spreads outside the prostate.
Staging
Staging of prostate cancer is a necessary step to determine the extent of the disease and select the best treatment strategy. A pathologist will look at the tissue that was taken during the prostate biopsy and will determine The size of the cancer area (percent of biopsy with cancer) The type of cancer cells The pathologist will assign a Gleason score based on how the cancer looks under a microscope. This score is an estimate of how fast the cancer is likely to grow and the life expectancy of the patient. In general, the lower the score, the better the prognosis.
2 to 4
Indicates tumors with cells that are expected to grow slowly and not spread rapidly.
5 to 7
Indicates tumors with cells that are moderately dispersed and are anticipated to grow with moderate aggressiveness.
8 to 10
Indicates tumors with cells that are likely to grow rapidly and metastasize (spread to other parts of the body). Most of the information listed above will appear on the biopsy report. The biopsy report (also known as the pathology report) typically has a diagram illustrating the cross section of the prostate. On the diagram, locations where tissue samples were collected will be indicated. These locations will be labeled either “no prostate cancer” or “prostate cancer”. Below the diagram is a table listing more detailed information of each sample collected. The samples are listed in the first column according to their location/site within the prostate. Other columns in the table list the length of the tissue sample collected, whether prostate cancer was found (Yes or No), the percentage of the sample in which prostate cancer exists, and the Gleason score. The Gleason score on the report may consist of two numbers (eg, 3,4). The first number is the grade assigned to the cancer type that is most numerous in the tissue sample. The second number is the grade assigned to the cancer type that is the second-most numerous. To determine the total Gleason score, these two numbers are added together. (See above for the interpretation of your score.) After all of the necessary tests are run and the results are available, your doctor will determine the stage of prostate cancer.
Stage I Cancer (also called T1)
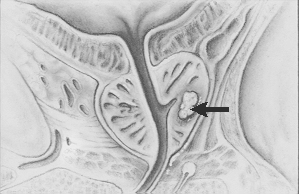
Stage II Cancer (also called T2)
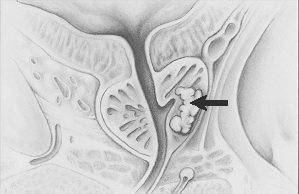
Stage III Cancer
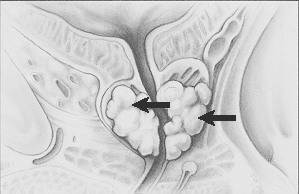
Stage IV Cancer
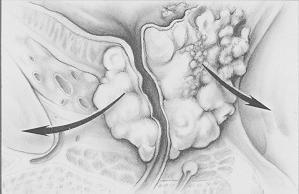
Risk Assessment
After a prostate cancer diagnosis and staging, you should familiarize yourself with the available risk assessment tools to help understand your risk of disease recurrence and progression.
The D’Amico classification system is one of the most widely used approaches for assessing prostate cancer risk. Originally developed in 1998 by Anthony D’Amico, MD, PhD, a professor of radiation oncology at Harvard Medical School and chief of the Division of Genitourinary Radiation Oncology at Brigham and Women’s Hospital and Dana-Farber Cancer Institute, this classification system is designed to evaluate the risk of recurrence following localized treatment of prostate cancer.
The system categorizes patients into three risk-based recurrence groups: low, intermediate, and high risk, using such measures as blood PSA levels, Gleason grades, and tumor stages via T-scores.
Function and Importance
The D’Amico risk group classification system was developed to estimate the likelihood of recurrence for any patient using a given set of parameters and is widely used as one of many individualized risk assessment tools. This analysis could help those battling prostate cancer to make a more informed decision regarding their treatment.2
By defining your prostate cancer as being part of one of these three groups, this system could potentially help you and your healthcare provider make more informed treatment decisions. There are many factors to take into account when making a decision regarding prostate cancer treatment, including long-term quality of life and other risk factors or chronic health conditions you may have.
All prostate cancer treatments carry some level of risk for complications or side effects. How serious these complications can be will vary from person to person, but are important to keep in mind when choosing a treatment plan
How Prostate Cancer Is Treated
How the System Works
First, it’s important to gather your numbers:
- PSA: The results of your PSA test, a blood test that detects prostate-specific antigen—a protein produced by the cells in your prostate
- Gleason score: The results of your Gleason score, given based on the microscopic appearance of your cancer cells
- Clinical stage T score: And your T stage, the size of your tumor as seen on an ultrasound or during a rectal exam
Using these numbers, your risk is either categorized as:
- Low risk: Those with a PSA less than or equal to 10, a Gleason score less than or equal to 6, or are in clinical stage T1-2a
- Intermediate risk: Those with a PSA between 10 and 20, a Gleason score of 7, or are in clinical stage T2b
- High-risk: Those with a PSA of more than 20, a Gleason score equal or larger than 8, or are in clinical stage T2c-3a.3
What the Research Says
Two studies that included more than 14,000 prostate cancer cases looked at the ability to predict cancer-specific and overall survival rates as well as the clinical relevance of such a risk-based classification system in contemporary medicine.
The studies estimated survival rates after surgery with a method called the Kaplan-Meier method. This analysis calculates the biochemical recurrence-free survival (BRFS), meaning survival from prostate cancer without a high enough PSA level to call it a cancer recurrence, rates in patients in varying stages of cancer. Those predicted survival rates were then compared to the actual cases to see if using the D’Amico risk-based classification system helped the patient make a more informed treatment decision and therefore increased chances of survival.
The studies found that men who had more prognostic information available to them (such as the D’Amico risk-based classification system) had overall higher survival rates following treatment for their prostate cancer, particularly those men with a high risk of recurrence.1
However, the system is not able to accurately evaluate the risk of recurrence in those with multiple risk factors. As prostate cancer cases with multiple risk factors are on the rise, the D’Amico classification system may not be as relevant to men with prostate cancer and their healthcare providers as other evaluation techniques.
What is risk assessment?
Prostate cancer can either present as a slow growing tumor causing minimal harm or a more aggressive type which spreads quickly. Risk assessment is the critical step of determining the nature of each patient’s disease. Physicians look at clinical and pathology features (PSA, Gleason score, clinical stage, etc) to determine which patients may have aggressive forms of prostate cancer, and which patients do not.
Risk assessment using clinical and pathologic information:
American Urology Association (AUA) groups (D’Amico classification): Patients are placed into risk categories based on clinical and pathologic features. The four groups are low (PSA 20 ng/mL, Gleason score 8-10, clinical stage T3a), and locally advanced very high risk (clinical stage T3b-T4)
Partin Tables:
predict the likelihood of the patient’s cancer being organ confined after surgery (i.e. pathologic stage)
Nomograms:
paper-based or online calculator methods that incorporate clinical and pathological information to provide risk assessment Newly diagnosed men become very familiar with their individual PSA and biopsy Gleason scores. Over the last several decades, annual PSA screening has helped identify more men earlier in the disease process. As a result, many patients present with a narrow Gleason score range (Gleason 6 or 7) and low PSA values which compress the results of existing risk assessment and prognostic tools, making them less useful for individual patients. New personalized methods of risk assessment using molecular biomarker analysis are available to assess progression risk.
Risk assessment incorporating molecular analysis as well as clinical and pathologic information:
Systems Pathology Approach (Prostate Px+):
analyzes the histology and molecular biomarkers from existing patient biopsy tissue with clinical information to provide personalized risk assessment Patients should learn as much as possible about their disease prior to treatment selection. Risk assessment and disease prognosis tools assist in making informed treatment decisions.
What to Expect
Learning more about prostate cancer and the available treatments is the first step towards improving your or your loved one’s outlook and relieving some of the anxiety and stress caused by diagnosis. Always get a second opinion. Research prostate cancer and treatment options. Read Us TOO’s Pathways for New Prostate Cancer Patients – brochure listing options for the newly diagnosed Request Us TOO’s free kit: Resource Kit for Making Prostate Cancer Decisions – kit of brochures & materials for the newly diagnosed. Visit Us TOO’s Online Communities: Prostate Pointers section for information on prostate cancer and its treatment. Jot down questions for your doctor. Ask about your doctor’s experience in treating prostate cancer. Bring along your companion, a family member, or a friend for support and an objective observer who can help translate what occurred in the doctor’s office. Once you or your loved one are diagnosed, your doctor will want to run tests and may need to ask you to have one or two imaging tests such as a bone scan or a computed tomogram (CT) or magnetic resonance image (MRI) to determine the extent of the disease. Depending on the stage of the cancer, the doctor will discuss treatment options. Certain treatments for prostate cancer are associated with side effects that can have a profound effect on one’s lifestyle. The important thing to remember as a patient is to keep a diagnosis of prostate cancer and the side effects of treatment from interfering with your life or your emotional health. Try to stick to your normal routine Eat a prostate healthy diet and enough calories to support your ideal weight. For a list of foods of prostate cancer food click HERE. Get plenty of rest. Pursue activities that are purposeful and meaningful – go back to work, play with your children or grandchildren Do things you enjoy – take a trip, go golfing Exercise regularly – it improves your physical and emotional sense of well-being. Anticipate changes in your lifestyle and find ways to accommodate them Incontinence (loss of urinary control) – sit at the back of the movie theater, sit on the aisle in an airplane. Erectile dysfunction – seek out sexual contact and reestablish intimacy. Seek out support from your family and friends. Join a support group for prostate cancer patients. For information about the Delaware Prostate Cancer Coalition’s support group, click HERE.
Questions For Your Doctor
The following is a list of questions to ask your doctor if you have been diagnosed with prostate cancer. It may be worthwhile to audio record your conversation with your doctor so that you can review his answers to each question and be able to make informed decisions about your treatment options.
After Diagnosis
What additional tests will I need? What is the stage of my cancer? Has my cancer spread and if so, how far? What are the treatment options for this stage of cancer? What are the benefits and risks of the type of therapy you are recommending? What side effects are associated with the type of therapy that you are recommending? What can I do to improve the success of my therapy? Are there other treatment options? Should I consider participating in a clinical trial? Can you refer me/us to a colleague who is not associated with this institution for a second opinion? Where can I find out more about my or my loved one’s treatment options? Where can I find advice about coping with the emotional impact of prostate cancer diagnosis and therapy? Are there any cancer support centers nearby?
Surgery
How many of these operations have you performed? What level of success have you had in preserving erectile function and/or continence in your patients following surgery? What can I expect following the surgery in terms of recovery time and short- and long-term side effects? What kind of follow-up can I expect after surgery?
Radiation Therapy
What type of radiation therapy will you be using and why? What level of success have you had in preserving erectile function in your patients following this type of radiation therapy? What can I expect following radiation therapy in terms of recovery time and short- and long-term side effects? What kind of follow-up is needed after radiation therapy?
Hormone Therapy
What type of hormone therapy do you recommend and why? What side-effects can I expect from this type of therapy? How long will I need to receive hormone therapy? What are my options in terms of continuous versus intermittent hormone therapy? Read a list of questions for urologists, radiation oncologists and medical oncologists, as compiled by an experienced prostate cancer patient View list of questions created by Prostate Problems mailing list participants
Finding Support
While the Internet has become a valuable source of information and support for those dealing with prostate cancer, it is recommended that you verify all information you obtain from the Internet with your doctor. Your doctor is a good resource who can give you information about prostate health and cancer, and who can direct to you other resources of support. Find a urologist. Also visit AUA’s Urology Health website for additional excellent information on adult conditions of the prostate. Find a medical oncologist in your area by consulting the American Society of Clinical Oncology (ASCO). Also visit ASCO’s website entitled People Living With Cancer for additional excellent information about prostate cancer. Find a local Us TOO support group chapter. The Us TOO mission is based on the Chinese proverb, “To know the road ahead, ask those coming back.” Talk to other men who have been diagnosed and treated, and/or speak to the wives and companions who are supporting their partners through their diagnosis, treatment and life after cancer. There are several national and international groups in addition to Us TOO that promote education about prostate cancer and its treatment, provide support, and act as advocates for prostate cancer awareness. Find a listing of them here

